How Busy Hospitals Can Increase Patient Flow: 7 Tips

The onset of the COVID-19 pandemic saw high volumes of patients, which drove many facilities to use new technologies and processes to accommodate the record numbers. Some hospitals still face significant patient loads that go beyond their capabilities, impacting patient flow.
While increasing patient flow might seem challenging, hospital leaders can deploy Internet of Things (IoT) technologies to improve efficiency in every department and prepare for challenges.
Ensure efficient daily operations and the highest level of patient safety and satisfaction with CenTrak Workflow™ solutions.
What Is Patient Throughput?
Patient throughput describes the movement of patients from arrival to discharge. It involves the care, resources, and decision-making to move patients through a hospital or healthcare facility. An optimized patient throughput process often improves the quality of care patients receive as well as their level of satisfaction with their experience.
Why Is Patient Flow Important?
Patient flow ensures patient safety and quality care. An effective patient flow process prevents overcrowded departments, poor handoffs, and delays in delivering healthcare.
By understanding and controlling patient throughput better, hospitals and their patients can expect these other benefits:
- Reduced wait times
- Improved patient care
- Decreased costs to the healthcare facility
- Improved staff satisfaction
- Increased productivity
In addition to improving existing workflow, preparing to open a new facility is a great opportunity to think through strategies and technologies to address workflow challenges.
At CenTrak, we offer patient flow software solutions to address a facility's unique needs. Oregon Medical Group partnered with us to implement a Real-Time Location System (RTLS) and integrated the technology with their electronic health record (EHR) system. To combat the issues that came with the unique layout of the new location, the software enabled patients to spend more time with their care team while experiencing decreased appointment wait times.
7 Tips to Optimize Patient Throughput
Every hospital can benefit from patient flow best practices— even minor improvements can make a meaningful impact. Here are tips for improving patient flow and creating a healthier, happier, and safer facility.

1. Increase Communication and Goals Across All Hospital Departments
Patient throughput must be addressed on a whole-hospital level. Every part of the hospital is connected and the cause of a patient flow issue or bottleneck may occur several steps before its noticeable effect. For instance, a patient flow problem in the inpatient units may result from issues with discharge procedures. Therefore, all hospital staff members, including nurses, physicians, and administrators, must understand the objective of improving patient flow and the processes required to accomplish related goals.
The first step to improving patient flow is to create a team. The patient flow team should include a representative from every department in the hospital. The team will then work to identify issues, set goals, and oversee changes.
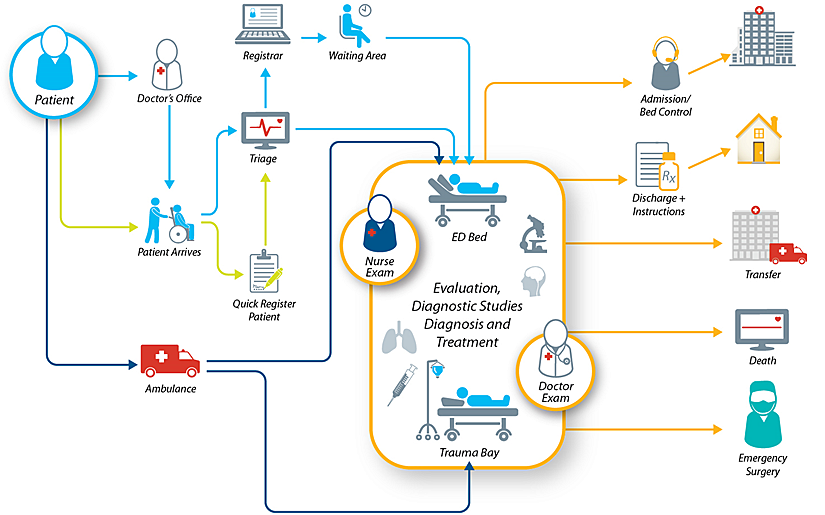
The team can start by drawing a patient throughput diagram to map the current design and measure performance. Team members should ask questions such as:
- Are there any bottlenecks with the current patient flow process?
- Are all the steps in the current flow necessary?
- How often do staff members complete each step?
- Can some of the steps be completed simultaneously?
- Is there a better way to sequence the steps?
- Can someone with fewer skills perform a particular step?
- What technology can be used to make steps easier?
After team members reflect on the current state of patient workflow and identify problem areas, they need to set goals. For example, the team might create a plan to improve communication between staff members. The hospital can adopt technology like CenTrak's RTLS to meet this goal. Our RTLS consists of wearables that can be attached to staff members and patients or medical equipment.
RTLS functions similarly to a GPS but can integrate with other healthcare technologies such as EMF and EHR systems. It provides real-time data and allows staff to automate clinical processes for a more efficient and hands-free approach to patient care. Additionally, hospitals can integrate the RTLS software with their nurse call systems for improved staff communication across departments. Nurse call automation allows instant alerts and increased response times.

2. Tighten up Non-Clinical Services That Support Patient Care
Non-clinical staff members or those who do not provide any clinical treatment or testing services significantly impact patient flow. These include staff members who fulfill roles in transportation, housekeeping, billing, and other administrative tasks. Management should evaluate non-clinical activities and find ways to improve their speed and efficiency. Here are efficiency-boosting tips for non-clinical services:
- Invest in training: All hospital staff require ongoing training to perform at their best. Staff training and education are worth the investment because they increase employees' confidence, keep them engaged, and enhance motivation. Training also improves their skills and increases patient satisfaction as a result. All of this helps staff members work more efficiently.
- Embrace technology: Use technology to automate as many processes as possible and reduce the need for manual work. For example, healthcare facilities can automate check-in and check-out procedures using self-service kiosks to eliminate bottlenecks. Another example is the use of RTLS with medical equipment. CenTrak's asset management solution with RTLS tracking software enables biomed staff to locate equipment quickly with real-time locations. This asset visibility can improve rounding workflows for preventative maintenance procedures and ensure critical equipment is always available when needed.
- Hire the right staff: When hospitals hire new employees, they want to select individuals who fit their values and care about patient satisfaction — not just the salary. It's worth waiting for the right candidate rather than focusing on filling a position. Suitable staff members want to be efficient and successful in their roles, all while providing excellent service.
3. Uncover Blind Spots With Real-Time Location Data
Healthcare professionals often leverage data from existing systems, such as EHR systems, to determine how long each step takes and develop ways to improve the workflow. However, this approach can unintentionally create blind spots. It can fail to account for time between the patient arriving in the exam or operating room and waiting for the provider.
The rest of the patient milestone steps are rarely recorded, resulting in a lack of transparency and clarity regarding patient wait times, patient-provider interactions, or the total visit time.
RTLS can help healthcare organizations uncover blind spots by automatically collecting patient throughput data in real time. Having a patient wear an RTLS badge during their visit is the only way to automatically collect real-time arrival-to-discharge data that is visible immediately and can be used by staff to modify the process as it's happening.
The secret to effective patient flow is balancing demand versus capacity and that's why being able to fine-tune processes with accurate real-time data is the optimal solution. Here are a few examples where RTLS can make a difference:
Multidisciplinary Ambulatory Practice
The arrival and registration process is crucial for keeping patient appointments on schedule. By using RTLS, a real-time queuing system can be implemented that creates an orderly, Health Insurance Portability and Accountability Act compliant registration and rooming process. It provides accurate arrival and registration wait time data.
Staff can now "see" that one of the patients waiting to register is here to see the only specialty practice that is "on time" with their schedule. Staff can pull that person ahead of the patients who arrived early for their appointments — keeping that practice's schedule on time. Simultaneously, staff can support the other practices and help them get back on track by adjusting schedules based on who is in the waiting room.
The Entire Patient Visit
RTLS will automatically measure patient wait times, notify staff of extended waits, and let practitioners know when their patient has arrived in the exam room and is ready to be seen. This real-time awareness of patients waiting for services and of patient readiness is like "turning on the lights," creating a more efficient experience for both patients and staff.
Hospital Radiology and Imaging Departments
These departments often provide services to both inpatients and outpatients. Offering real-time knowledge of outpatient arrivals and the location of inpatients needing radiology exams and imaging studies gives radiology and imaging technologists valuable information — and allows them to maximize their delivery of services while minimizing the wait time for all patients.
Operating Room (OR)
One of the most pivotal transitions for patient throughput is the OR turnaround time (TAT). Staff documentation is unlikely to measure the actual time between wheels-in and wheels-out accurately. Documentation also does not measure the time spent by each staff type involved in turning over the room.
RTLS can measure this much more accurately while notifying turnover team members when the patient has left the surgical suite and is prepared for cleaning and alerting the surgical team when the suite is ready for the next patient. It also offers an opportunity to keep a patient's family updated on the progress through the surgical experience — all in an automated way and delivered to visual boards in waiting rooms or via secured text messages to family members' mobile phones.
By automating this value-added step, hospitals directly reduce the burden on staff who had to previously track that information and make multiple phone calls to provide status updates.
Communicable Diseases
Diseases such as COVID-19 call for healthcare organizations to redesign their workflow processes to limit the potential exposure to pathogens, especially in spaces where people congregate, such as registration areas and waiting spaces. A transition from a physical waiting environment to a virtual waiting room, with contactless check-in and self-rooming, is now possible by leveraging Real-Time Location Technologies.
Contact Tracing
RTLS data is also a critical tool for contact tracing, as it enables efficient and thorough reporting on interactions among people. When staff and patients wear RTLS badges, all patient and staff contact that occurred in the same location, along with the duration of contact time, are monitored. This data enables healthcare organizations to promptly take any necessary follow-up action for patients and staff, such as isolation, symptom monitoring, and prophylactic treatments if appropriate.
4. Track and Streamline Cycle-Time Measurements
Cycle time measures how long it takes for any process or combination of processes in the hospital to occur. For example, the amount of time it takes a patient to be registered, receive treatment, and be discharged from the hospital. In the United States, patients wait over an hour and a half to be taken to a room in the emergency department (ED) on average and over two hours before they get discharged.
As efficiency increases, cycle time decreases, and patient throughput can be increased to meet demand, thus reducing the need for additional resources. In contrast, poor departmental processes can lead to long cycle times, impacting patient outcomes and patient satisfaction.
As a first step to reducing the cycle time in the Emergency Department, leaders should follow the flow of a patient's journey through the ED. Use streamlined tracking tools such as RTLS to gather real-time patient throughput data automatically. With RTLS, hospitals can follow patients from check-in to check-out and identify bottlenecks and inefficiencies at every stage. They can see exactly how long a patient spends waiting in each area. For example, a hospital manager using location data as a reference might notice a long wait time in the radiology department. They can use this RTLS data to take steps to remedy the problem.
Here are more tips to reduce the cycle time:
- Staff to meet the demand: If patients have the choice, they will likely visit the ED in the evening or on weekends when they don't have to miss work. However, physicians and nurses may prefer working during weekdays. To reduce cycle time, regularly monitor the volume of patients in the hospital and ensure that the ED has enough staff to meet the demand.
- Ensure supplies and equipment are easy to find: Staff should not waste time looking for medical equipment or supplies. Any inefficiency in the cycle can lead to a bottleneck. Hospitals can use asset tracking to increase visibility to show staff the exact location and condition of critical resources.
- Improve the registration process: Patient registration is a necessary step that should not create delays in care. Consider the number of steps in the registration process as patients check in and how long each step usually takes. Hospitals can reduce check-in time by asking the minimum amount of questions needed to identify the patient and collecting more information at the bedside. Other solutions include self-check-in/registration. Upon arrival, patients are given a device or use their own to complete a patient intake application. The information can be pushed directly to the EHR and other technology integrations, such as RTLS, for a seamless flow of information.
5. Improve the Hospital Layout
Considering the layout is an excellent way for the emergency department to increase patient flow. The layout should make it as easy as possible for staff and patients to navigate the facility and complete tasks. Here are tips to improve the layout and promote flow:
- Display easy-to-read signage: Be sure the hospital clearly leads staff and patients through the parking lots, lobby, and various departments. Consider our digital wayfinding solution, which features turn-by-turn navigation, highlighted routes, and custom routing. These solutions make it easy for patients to navigate the hospital through a mobile app. When hospitals keep patients from getting lost, the number of late or missed appointments is reduced.
- Flow in sequence: Many times, patients check in, take a seat in the waiting room, and then have to cross paths with other patients to go to an exam room. Make sure the layout supports the flow of events as they happen so patients do not have to cross paths with others or retrace their steps. Be sure to use separate check-in and check-out areas as well. Consider solutions such as self-rooming procedures and immediate notifications to staff on who is waiting, where, and for how long. This eliminates the need for clinical staff to go back and forth between floors and areas of the department or facility to retrieve patients from a central waiting room.
- Provide stand-up workstations: Place stand-up workstations in a central area to give doctors and nurses quick and easy access to the EHR system. Medical staff should not have to travel far to take notes or review records before moving on to the next patient.
- Place supplies in patients' rooms: Keep essential supplies in easy-to-reach storage drawers in patients' rooms so staff have access to resources when needed. Hospitals might also keep supplies in a central area or well-stocked mobile carts. Managers must consider storage solutions that would provide the most convenient access, depending on their unique needs. It helps to ask staff members for their opinions.
- Offer more outlets: Staff members may use mobile devices to access the EHR and patient information and they shouldn't have to search for outlets or USB charging stations to keep their batteries full. Ensure enough outlets are available in the layout or furniture so staff does not have to waste time when their batteries get low.
- Divide rooms into areas: The entrance of patients' rooms should provide open space for staff to perform their tasks. The beds should be kept in the center of the room, and visitor seating areas should be in the back. This layout helps staff members enter and exit rooms freely as they provide patient care.

6. Train Hospital Staff on Time Management
Be sure every staff member in the hospital is taught time management techniques. Time management is the process of planning how one uses their time to increase efficiency and productivity. Everyone, from receptionists to physicians, can benefit from improving their time management skills.
For example, hospital leaders might emphasize the importance of using technology to save time. Hospitals might introduce new technology, such as RTLS, to help staff members manage their time better. Training staff on using new technologies and giving them the support they need to use these tools effectively is crucial. Here's how hospitals can help staff embrace changes that improve time management:
- Let the staff know ahead of time so they can prepare for the new technology and the change in their routine.
- Talk to the team about the benefits of technology and how it will ultimately make their jobs easier and improve patient care.
- Ensure staff understands that tools like RTLS are not meant to monitor them for disciplinary purposes but are there to improve patient flow.
- Hold regular meetings to discuss the purpose of new communications or monitoring systems and address any issues or concerns staff members might have.
7. Utilize Data Analytics to Make Efficient Decisions
Thanks to our patient flow management technology, healthcare professionals can use a range of devices and software to collect and analyze data, such as EHR, online patient portals, and location devices. These tools offer valuable insights for managers making informed decisions to improve patient care, support staff, and increase efficiency. Managers can also use the information to show staff the impact of their work on the hospital. With task automation in healthcare settings, monitoring patient workflow and identifying potential inefficiencies becomes easier.
Increase Patient Flow in Hospitals With CenTrak
When patients visit a hospital, they should feel cared for, safe, and appreciated. Staff should feel confident they have the resources, skills, and time to provide the best care possible. Technology like CenTrak's RTLS helps reduce stress and simplify tasks for staff so they can focus on what matters most: patient care.
Hospital managers considering RTLS should reach out to CenTrak. CenTrak offers robust, easy-to-implement RTLS technology to improve patient throughput and employee satisfaction. With CenTrak, hospitals and healthcare facilities can reduce costs and increase efficiency as patient volumes continue to grow. To learn more, request a demo or contact us today.